The news headlines over the past few years have been the most bizarre of my lifetime. You can’t make this stuff up. First there was this weird virus called COVID-19 which turned healthcare upside down. Then they were telling us about the Murder Hornets which sounded absolutely terrifying. Now, we are hearing about this monkeypox disease and I’m just about over it. Are you kidding me? What the heck is it and do I need to be afraid? Let me take a moment to discuss it and get you the facts in an understandable way.
What causes monkeypox?
Monkeypox is caused by the monkeypox virus, a member of the Orthopoxvirus genus. This family of viruses has not been a recent problem for us as humans. The only other Orthopoxvirus you may have heard of is smallpox which was declared eradicated in 1980 secondary to the world vaccination initiative in the 70s. Monkeypox looks like smallpox in presentation, but it is much less severe.
Where did monkeypox come from?
Monkeypox has been around for many years, but it hasn’t been a global problem. It has primarily been staying in the rainforest regions of western and central Africa. It’s a natural occurring virus in non-human primates, rodents, and squirrels. Every few years, a small outbreak has occurred in humans, and the experts believe this was due to direct contact with one of these animals. Most likely, people became infected from cleaning these animals for consumption or eating undercooked meat.
When a virus jumps from an animal to a human, that process is called zoonosis. You might hear something about this being a zoonotic disease. Try to work zoonosis into your lunch group tomorrow and look at how smart you’ll appear. You’re welcome.
So now we have an understanding that this disease looks like smallpox, but isn’t as serious, and that it came to humans from infected animals. Got it. But then why is this 2022 outbreak different and why are we hearing so much about it now? Prior to this year, the cases of monkeypox were primarily traced back to an infected human being in contact with an infected animal. The number of cases of human-to-human contact were pretty rare. For whatever reason, this outbreak has been spreading rapidly across the globe in primarily human-to-human contact. As with most viruses, there was likely a mutation that made it more transmissible.
To date there are about 50,000 cases worldwide and about 18,000 of those are in the US.
Will I get infected? How does monkeypox spread?
When I was asked this about COVID the answer was “Yes, you likely will get this disease because it is highly transmissible,” and most cases were being transmitted before people even had any signs of disease. This isn’t the case with monkeypox. The primary spread of monkeypox is from direct skin-to-skin contact with the fluid inside the rash itself.
It’s possible that people are inhaling large respiratory droplets, but the experts are still trying to see if this is true. These droplets could be from somebody talking or coughing in your face. Contact tracing is going on as we speak, but the majority of cases by far have been skin-to-skin contact. And to even narrow it down further, the CDC says that the majority of those skin-to-skin contact cases have come from gay, bisexual, and other men who have sex with men.
So, what do the symptoms of monkeypox look like?
For those of you who have seen chickenpox, monkeypox looks a lot like it.
There is no relation to chickenpox other than the look and feel, but if a patient came in with this rash last year, they would have likely been diagnosed with chickenpox while waiting on confirmatory testing. They are large painful blisters and when you see this rash, most of us know to try to avoid contact with pregnant women, those with lower immune systems (like cancer patients and those with uncontrolled HIV), and children. Also, like chickenpox, we tell folks to avoid other human contact until the blisters have scabbed over and new skin is starting to appear.
How does monkeypox progress?
The stages of this disease are quite fascinating as well. In the first stage of illness, often called the “prodromal phase,” the patient may have a fever, headache, body aches, swollen lymph nodes, chills, and exhaustion. If a patient were to come in without the rash and these symptoms right now, we would work them up for flu, strep, COVID, etc. However, a few days later the rash starts to appear.
The rash has a very predictable pattern of development. The first blister, or vesicle, comes up almost looking like a standard pimple. It then has this “divot” in the middle which we call umbilicated. Then you will start to see some black areas on the blister called an eschar. That’s the scab you hear people talking about. Patients are infectious during all the stages of the rash. Once the scab falls off and new skin is growing, they’re no longer contagious. This next picture goes through all these stages starting at the upper left to right and then bottom left to right.
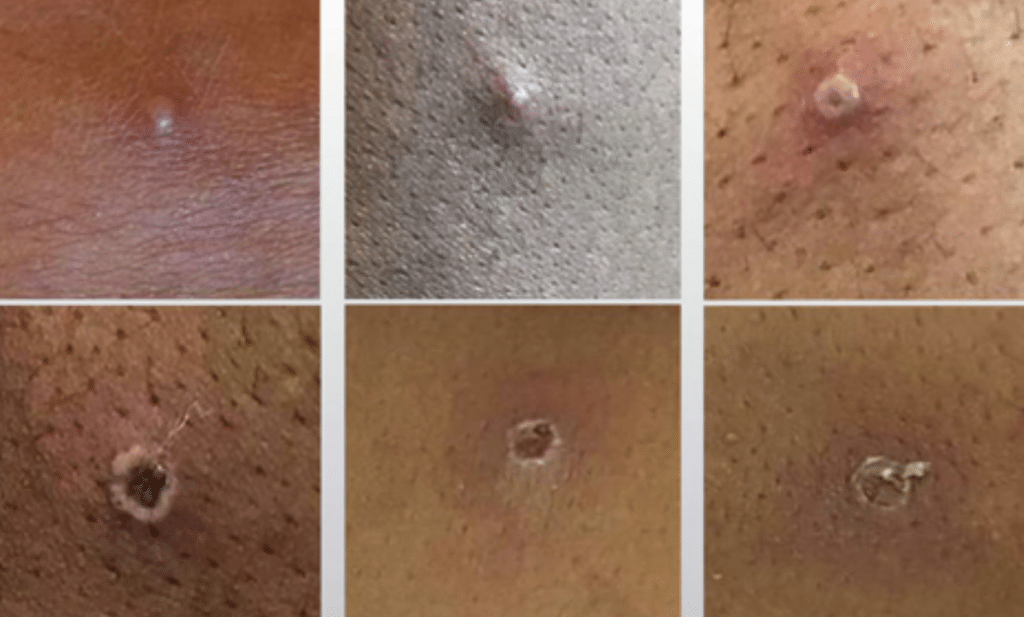
So, if this is primarily passed through skin-to-skin contact with the rash, it should be fairly obvious if I need to be on the lookout for getting this illness, right?
You’re mostly correct. It is the fluid inside the vesicle that is contagious. So, you really need to be in direct skin-to-skin contact where the vesicle breaks, and the fluid then gets in contact with your body. Scientists are still investigating if this Monkeypox virus can be transmitted by non-contact such as being in close contact talking to an infected person or them coughing in your face. That is why the CDC is recommending mask use around folks infected and those who are in close contact with them.
How long after contact with somebody with monkeypox should I be concerned that I may get it?
The incubation period for monkeypox is 5-21 days. So, if you were around somebody that was diagnosed with the virus you need to be wearing a mask and limiting your contact with others for 21 days. If you have not noticed a rash after this period, you are considered not contagious. The CDC has broken exposure risks down into:
High Risk – Direct BROKEN skin-to-skin contact with an infected individual with the rash or possibly being in the patient’s face for prolonged periods (greater than three hours) of time where they were breathing or coughing directly in your face.
Medium Risk – Direct skin-to-skin contact with INTACT skin lesions of an infected individual or being around the infected person for less than three hours.
Low Risk – Being around somebody who has monkeypox for less than three hours.
So, what do I do if I think I may have it?
Call your doctor and get an appointment and let them know you are concerned for monkeypox and make sure they can test for it. At Xpress Wellness Urgent Care and Integrity Urgent Care, we have already tested and diagnosed several cases of monkeypox. The test is pretty straightforward and simple. We swab the blister until it opens and send the fluid off to the lab to be tested. We have folks quarantine until the lab results come back. This is a reportable condition and therefore we report the positive cases to the local health departments so that contact tracing can be performed.
So, what do I do if my test comes back positive for monkeypox?
We all sort of got beat over the head about quarantining during the COVID pandemic, but here it goes again. You are supposed to isolate as much as possible and wear a mask if in a house with others who can’t live elsewhere. You stay in quarantine until the rash scabs over and new skin is starting to grow. This typically takes about three weeks from beginning to end.
By and large, the treatment is just to let the virus run its course while you quarantine. You can take Tylenol and ibuprofen for pain. There are a few patients that may qualify for an investigational treatment called Tpoxx. This is a medicine that must be requested from the CDC from the Strategic National Stockpile (SNS) and very few people qualify. It comes in a pill and IV form and is reserved for those with really severe symptoms or those who are at very high risk for bad outcomes. Your medical provider will know if you need this medicine. If you are prescribed Tpoxx, you can’t just go to your local pharmacy and get it. It will be sent to you from this SNS.
So, what do I need to do to protect myself?
The best protection you can have is not being in close contact with somebody who has monkeypox. This is possible in the vast majority of cases. If you have been in contact with somebody inadvertently, do your best to isolate yourself for twenty-one days. Avoid going to crowded places where intimate skin contact could occur such as raves and crowded concerts. Absolutely avoid intimate skin contact with any other individual with a blister-like rash.
Should I take the monkeypox vaccine I hear about in the news?
There are two vaccines that are being used under emergency use authorization. If you were vaccinated against smallpox, you’re likely already protected. If you are at high risk because of frequent encounters with individuals with the virus then talk to your healthcare provider about getting the vaccine. Some individuals qualify for PEP (Post exposure prophylaxis) which means getting one of these vaccines after exposure. This is usually coordinated with your local health department and reserved for those with high risk and sometimes medium risk encounters.
There’s a national shortage of these vaccines, and health departments are being very selective of who needs to get this vaccine. As a health care provider myself, I do not qualify for this vaccine nor is it necessary for most healthcare providers. In fact, I was in a lecture with an infectious disease doctor this week who is the referral source for many of these positive monkeypox cases, and even she isn’t taking this vaccine. She is wearing normal clothing that covers her skin and a mask when encountering these patients and she feels this is all she needs.
Okay, so should I be worried about monkeypox?
In summary, monkeypox is a viral disease that is primarily spread through intimate skin contact with other individuals that have the virus. We don’t need to be afraid and can usually avoid any contact with infected individuals through normal precautions. If you have been in contact with someone who tests positive in a medium or high-risk situation, quarantine for twenty-one days and if no rash develops, you are good to go.
If you happen to contract the virus, just realize it is more than likely self-limiting, and your only treatment will be to quarantine until the scabs are falling off and fresh skin is growing. There will be a very small subset of people who are at risk for truly getting very sick by this disease and that subset of individuals will be guided through the process of receiving treatment plus or minus the vaccine.
Thank you for going through this exercise with me and feel free to visit any of our clinics to get tested if you have a rash that doesn’t seem right to you. Continue to make educated choices about your healthcare and let us know if we can help you along the way.
Thank you,
Dr. Eddy Dark
El Director Médico Asociado
Xpress Wellness Urgent Care / Integrity Urgent Care






